“Of all the forms of inequality, injustice in health care is the most shocking and inhuman because it often results in physical death.” Dr. Martin Luther King Jr.
Despite growing recognition of the quality gaps in health care access and delivery in the United States, health disparities persist and we continue to lag behind other developed countries in key health outcomes. In our quest to train the future healthcare workforce to be committed, compassionate and responsive to the needs of our diverse and evolving patient populations, the University of Illinois at Chicago (UIC) College of Medicine offers the Patient-centered Medicine (PCM) Scholars Program, one of the first in the nation to explicitly train health science students to practice patient-centered care. The development, implementation and lessons learned from our journey in the continuum of campus-community partnership building and training health profession students in humanism, social justice, advocacy, leadership and scholarship to address health disparities span over a decade and a half. We have established partnerships with Chicago Area Community Agencies serving six especially vulnerable groups: the elderly, persons living with HIV/AIDS, the homeless, immigrants/refugees, survivors of intimate partner violence and incarcerated persons. Our uniprofessional teaching and learning journey started with medicine and is now interprofessional, including dentistry, nursing, pharmacy and public health.
In 2005, with funding from American Medical Student Association (AMSA), we developed the first Service Learning Program for UIC College of Medicine to prepare the future healthcare workforce to address health inequities and disparities. This was the forerunner to the Patient-centered Medicine (PCM) Scholars Program which was initiated in the fall of 2007 as a Health Resources and Services Administration (HRSA)-funded, longitudinal continuity of care curriculum. The program spans undergraduate medical training and aims to inculcate in learners the attitudes, values and competencies necessary for providing patient-centered care.
A central thread is the students’ involvement with continuity patients. (Figures 1 & 2).
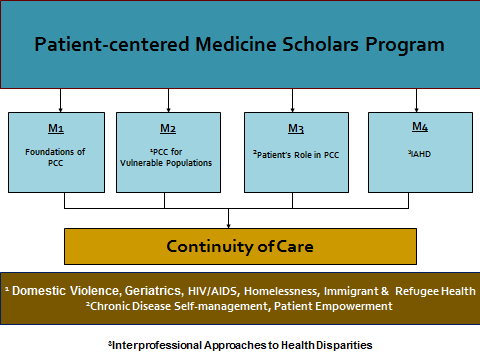
Figure 1: Figure 2:
Figure 1: Model for Patient-centered Delivery of Care Figure 2: PCM Scholars Program Structure & Organization
Active experiential learning, reflection, application and integration are vital pillars of the curriculum. PCM Scholars Program fosters the development of critically reflective future health professional leaders and scholars who embrace the concepts of patient advocacy, humanism, empathy, compassion, and blend it with the art and science of medicine. The program has a special focus on patient-centered care for vulnerable populations, training PCM scholars to take into account social determinants of health and preparing them to address health disparities.
In 2013, through a Josiah Macy Jr. Foundation Faculty Scholars Award, we developed the “Interprofessional Approaches to Health Disparities” (IAHD) course which was integrated into the M4 (4th year) component and provides an opportunity for medicine, nursing, pharmacy and public health students to work in teams on community-based participatory research projects. Dentistry joined the program in 2019. In this mentored interprofessional learning environment, future health professions leaders acquire skills to effectively address the rising burden of key public health concerns. Our work is a continuum of campus-community partnerships to train health science students to address health disparities via interprofessional collaborative education and community-based participatory research (CBPR), grounded in the common pathway of social determinants of health. Trainees work in interprofessional teams and engage in a series of didactic and experiential learning activities. A substantial element of learning includes training in CBPR methodology and hands on work with vulnerable persons and staff at community agencies to develop and carry out CBPR projects using the Plan-Do-Study-Act (PDSA) framework for incremental change and quality improvement. Program evaluation indicates that learners view the learning experience positively. An important lesson from this experience is the reminder that designing and implementing interprofessional education is not an easy task. There are several lessons we have learned through our journey of program development and implementation. Below are some key lessons we continue to pay heed to as we proceed.
- When people start working individually and in silos, there is a lot of wasted energy and resources. Hence, it is critically important to get people engaged early on to work together collaboratively.
- Theory and evidence need to be integrated in curriculum transformation efforts. We have drawn heavily from theoretical and conceptual frameworks, such as Kotter’s principles of change management and Kern’s principles of curriculum development. We use these as conceptual frameworks and core foundation for developing IPE at our institution.
- Curriculum development should be responsive to local, regional and national trends and emerging needs in health professions education and health care delivery and practice.
- Involving student input is essential in developing learner-centered and meaningful educational programs.
- The “interprofessionalism” of any IPE program includes faculty as well as students. Recruitment and development of an interprofessional faculty group improves the likelihood of program sustainability as well as acting as an impetus for other collaborative IPE projects. Proactive recruitment and faculty development efforts are necessary to ensure widespread participation in interprofessional activities.
- Scholarly work must be central to program development and should be made a priority.
- Institutional support is crucial in providing the necessary infrastructure and support for program development, growth and sustainability.
- Successful teams thrive when there is trust, respect and shared goals and values. Our IPE team has been successful in collaborative program development, scholarship (papers, presentations), obtaining grant funding, and developing a network of mutually-supportive colleagues and friends.
- Finally, developing anything that is complex and multilayered can be both an exhilarating and exasperating experience. This is certainly true of curriculum development and charting into new territory, such as interprofessional education. Remembering what a great privilege it is to be a part of positively influencing the learning of our future health professionals is an ongoing extrinsic motivator for our team; when you do something with love, joy and gratitude it is so much better!
Our program is making meaningful contributions to advancing the health professions education science towards discovering new models for training the future healthcare workforce to address the needs of our evolving patient populations and to reduce health disparities. The work is grounded in a moral compass that calls for social accountability of academic health centers and expanding the training of our future health workforce to heighten health professions students’ personal commitment to service, social justice, and civic responsibility.
The PCM Scholars Program is an exemplar of John Dewey’s concept of “Education in Action”. The program fosters the development of critically reflective future health professional leaders, scholars and change agents who embrace the concepts of patient advocacy, humanism, and compassion, and blend it with the art and science of their health professions. Approximately 25% of PCM graduates choose to serve as primary care physicians. More importantly, 65% of graduates with PCM training experience choose residency practice locations in medically underserved areas. Students’ reflections about their experiences are available as “PCM Voices“. Long term, this work will continue to focus on bridging the gap between interprofessional education and practice and creating educational innovations responsive to the need for a highly trained healthcare workforce that is capable of meeting the challenges of the 21st century.
“Together we can do so much.” Hellen Keller
-Memoona Hasnain, MD, MHPE, PhD, Community of Practice Member
Dr. Hasnain is a tenured Professor and Interim Department Head in the Department of Family Medicine, College of Medicine, University of Illinois at Chicago (UIC). The primary focus of Dr. Hasnain’s work is at the intersection of medicine and public health, with an emphasis on humanism, empathy, social justice, health equity, interprofessional education, service and scholarship. She is a nationally recognized expert on health disparities. Dr. Hasnain has received numerous accolades for her research and teaching and is a recipient of the prestigious Macy Faculty Scholars Award by the Josiah Macy Jr Foundation. This award is given to select educators nationally to accelerate needed reforms in health professions education to accommodate the dramatic changes occurring in medical practice and health care delivery.
ACKNOWLEDGEMENTS
This work is contributions of a large number of individuals – faculty, students, staff, UIC Health Professional Colleges and our community partners.
Interprofessional Faculty
- Susan Altfeld, MA, PhD- Public Health
- Valerie Gruss, PhD, APN, CNP-BC- Nursing
- Memoona Hasnain, MD, MHPE, PhD – Program Director- Medicine
- Sarah Henkle, MD- Medicine
-
Keia K Hobbs, MD- Medicine
-
Jennie Jarrett, PharmD- Pharmacy
-
Mike Koronkowski, PharmD- Pharmacy
-
Sonia Oyola, MD- Medicine
-
Laura Amanda Perry, MD- Medicine
-
Nimmi Rajagopal, MD- Medicine
-
Patrick Dean Smith, DMD, MPH- Dentistry
-
Griselle Torres, DrPH, MPH, MSW- Public Health
-
Susan Walsh, DNP, APRN, PNP-PC- Nursing
- Connections for Abused Women and their Children (CAWC)
- Project Vida; EdgeAlliance/AIDSCare Progressive Services
- Lincoln Park Community Shelter; Cathedral Shelter (now Revive)
- Housing Opportunities and Maintenance for the Elderly (H.O.M.E.)
- Syrian Community Network, Heartland Alliance
- Juvenile Temporary Detention Center (JTDC)
Funding: Josiah Macy Junior Foundation; American Medical Student Association [AMSA]; Association for Prevention Teaching & Research [APTR] & CDC; Grant # 1 D56 HP 08344 by the Health Resources and Services Administration; UI-COM Department of Family Medicine
SUGGESTED READINGS
- Institute of Medicine. Committee on Quality Health Care in America. (2001) Crossing the Quality Chasm. A New Health System for the 21st Century. Washington, DC: The National Academies Press.
- Institute of Medicine. Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care. Washington, DC: National Academy Press; 2002.
- Hasnain M, Koronkowski MJ, Kondratowicz DM, Goliak KL. Training future health providers to care for the underserved: a pilot interprofessional experience. Educ Health (Abingdon). 2012 Sep-Dec;25(3):204-7. doi: 10.4103/1357-6283.109790.PubMed PMID: 23823641.
- Hasnain M, Massengale L, Dykens A, Figueroa E. Health disparities training in residency programs in the United States. Fam Med. 2014 Mar;46(3):186-91.
- Frenk J, Chen L, Bhutta ZA, et al. Health professionals for a new century: transforming education to strengthen health systems in an interdependent world. Lancet. 2010 Dec 4;376(9756):1923-58. doi: 10.1016/S0140-6736(10)61854-5. Epub 2010 Nov 26. PubMed PMID: 21112623.
- Josiah Macy Jr. Foundation. Macy Faculty Scholar Memoona Hasnain on Teaching Health Disparities. Available at: https://macyfoundation.org/news-and-commentary/memoona-hasnain-health-disparities
- Josiah Macy Jr. Foundation. Revisiting the Medical School Mission at a Time of Expansion. 2008. Available at: https://macyfoundation.org/publications/conference-summary-revisiting-the-medical-school-educational-mission-at-a-t
- Accessed, March 29, 2019
- Interprofessional Education Collaborative, IPEC, Core Competencies for Interprofessional Collaborative Practice: 2016 Update. https://hsc.unm.edu/ipe/resources/ipec-2016-core-competencies.pdf
- World Health Organization. WHO report: framework for action on interprofessional education and collaborative practice. 2010. Available at: https://www.who.int/hrh/resources/framework_action/en/ Accessed, March 30, 2019