Most medical professionals can readily recite the four core principles of bioethics: autonomy or respect for persons, beneficence, non-maleficence, and justice. Yet the field of bioethics has been criticized for the lack of attention to justice, in both clinical and scholarly spaces. Four years ago, an opportunity arose to rectify that within the undergraduate medical curriculum at SUNY Upstate. The entire institution was undergoing curriculum renewal, and “integration” was the buzzword. Existing first-year courses in ethics, law and social issues, and in population health and preventive medicine were well-received, but they were isolated and disconnected from the rest of the students’ coursework. And although they each relied on distinct discipline-specific tools, they shared important areas of content, including dual sessions on cultural humility, healthcare finance, advocacy, and global health.
The merger of the courses into one, now called Patients to Populations, presented several advantages. With increased contact hours (roughly 70 total in-class hours, as of 2019), the course no longer had to be squeezed into one or two organ-based units. This short-term schedule had unintentionally reinforced student perceptions that social medicine took a backseat to medical science, and was something that only mattered to a passionate few. As a longitudinal course, it better emulated real-world clinical practice—in which clinicians are constantly challenged to consider all of patients’ needs simultaneously. Small group discussions, which had been led in the past by pairs of faculty from the same department, were now led by faculty partners with complementary expertise, giving students an interprofessional and transdisciplinary perspective.
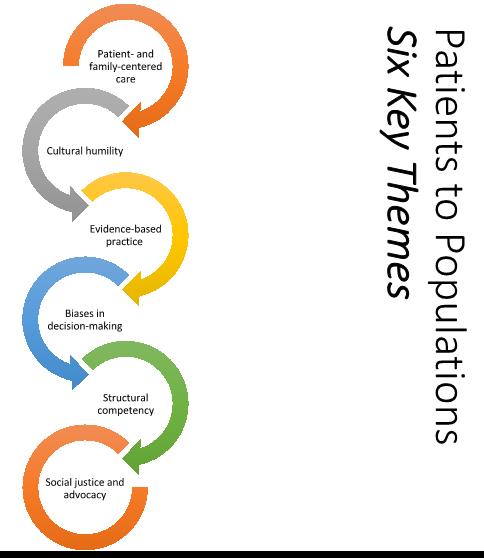
Concurrently with the development of Patients to Populations, the curriculum moved toward greater emphasis on case-based and self-directed learning. Bioethics had previously been presented as a series of lecture followed by 90-minute small group discussions. With the new course, students were now able spend most class time in the small group setting. We developed an innovative series of cases—stories, really—designed around six interrelated themes (see figure below). Each case opens with an encounter between a patient and a doctor, a deliberate decision made because our students are future doctors, and we wanted them to begin developing a professional identity while also practice crucial perspective-taking skills. As the case unfolds, a problem or dilemma reveals itself. Faculty choose when to share the next “event” in the narrative based on the students’ discussion and analysis. Each case is deliberately designed to elicit assumptions and then challenge those assumptions. Students are asked to own their biases, recognize and acknowledge their emotional reactions…and then to learn how to question, engage with and ultimately move past them, toward better care for patients. By the end of each case, students are grappling with the community and societal implications of situations like the one their hypothetical patient faces. They are encouraged to reflect critically on their obligations to advocate for policies that might help their patients lead healthier lives and to brainstorm ways they might do just that, for instance through research, community development, or legislative change.
This approach is not without its challenges. Students who, in past years, might have enjoyed 6 weeks of bioethics as a respite from the rigors of biochemistry, anatomy and physiology now have to learn how to balance the omnipresent pressures of the USMLE Step 1 examination with a year-long dive into bioethics, law, epidemiology, biostatistics, anthropology, sociology, health economics and public policy. The structure of the course and the rigorous assessment schema necessitate that students take learning this content seriously—showing up is essential but it’s not sufficient to pass the course.
There is no opting-out, either. Case discussions address racism, poverty, violence, and other topics that can be uncomfortable. At the start of each academic year—later this week, in fact—we review five expectations for students:
1. Listen and engage.
- Listen to your peers and engage with each other.
- Respectfully disagree and challenge each other.
- Critique ideas and positions, not people.
- Explain the relevance of issues when it is not obvious to your peers. Students enter medical students with greater variation in prior exposure to the issues taught in this course. Everyone is here to learn.
2. Make space, take space.
- Understand that we have a limited amount of time and every case represents a subject that people have devoted their lives and careers to addressing.
- Sometimes the discussion will move on before you’ve expressed all your ideas.
- Feel free to e-mail your facilitators or talk with them after class. Or continue the discussion with your peers!
- Be concise and give others time to speak.
- Only repeat a point when you have something to add.
3. Be humble.
- Listen to your facilitators.
- Medicine is rarely black and white but sometimes you will say things that are simply wrong and you will be corrected.
- Your facilitators have unique perspectives and experiences to share.
- Ask for clarification when you don’t understand.
- If a reading, topic or activity seems irrelevant à talk about with facilitators and course directors.
- Be open to the possibility that you may only appreciate its significance later in your career.
4. Bring yourself.
- Bring your previous knowledge and experiences, as well as the knowledge you are acquiring in basic sciences, to bear on the discussion when relevant.
- Be open: If your cultural or religious beliefs, your previous career, the fact that you are a parent or have a sick family member affect how you see a case, then this is the place to talk about it!
5. Raise the bar.
- Raise the bar throughout the year: push yourself to think more critically and express yourself more articulately.
- Use evidence and logic when challenging others’ assertions and ideas.
- Be willing to change your mind when others demonstrate errors in your evidence or logic.
- The quality of the dialogue in May should be much more nuanced, sophisticated, and informed by theories and principles in bioethics and public health than the dialogue in September.
Of course, these are not a panacea for all the difficulties of teaching medical students to recognize and confront injustice. We have still struggled with concerns about politicization of certain subjects (e.g., how to respond to a student request for a debate on whether EMTALA should apply to undocumented immigrants) and complaints regarding student comments perceived by peers as racist. Faculty development workshops have addressed concerns that female students were disproportionately interrupted by male students (solution: consistent enforcement of hand-raising rules) and that faculty were unprepared to talk frankly but sensitively about sexual violence. Our student body, diverse in many ways, is still primarily able-bodied, and that lack of perspective shows in our discussions of disability.
Little by little, however, our approach has become a central part of the first-year experience at SUNY Upstate. Next year, the first group of students to take the course will graduate and scatter across the country for graduate medical education and we may finally be able to learn something about the long-term impact of our approach. Do our students maintain a broad view of bioethics, with justice front and center? Are they better equipped to apply understanding of social determinants of health in clinical practice? Have they incorporated the values of our course into their professional identities? Will they serve underserved patients when they leave residency?
-Amy Caruso Brown, MD, MSc, MSCS, NCEAS Community of Practice Member
Dr. Caruso Brown is a tenured Associate Professor in the Center for Bioethics and Humanities of the Department of Pediatrics, Division of Pediatric Hematology/Oncology at SUNY Upstate Medical University. At Upstate, she directs the Ethics and Professionalism thread in UME and designed and directs Patients to Populations, a justice-centered bioethics course for first-year medical students. The curriculum was recently published as a textbook by Springer Nature. Her research interests include evaluation and assessment in social determinants of health education; pediatric disagreements; and ethical issues related to social media in pediatrics.
Further Reading:
- Caruso Brown AE, Hobart TR, Morrow CB, eds. Bioethics, Public Health, and the Social Sciences for the Medical Professions. 2019; Springer, Cham.
- Childress JF, Beauchamp TL. Principles of Biomedical Ethics. New York: Oxford University Press; 2001.
- Cruess RL, Cruess SR, Boudreau JD, Snell L, Steinert Y. Reframing medical education to support professional identity formation. Acad Med. 2014;89(11):1446-1451.
- Holm S. Not just autonomy–the principles of American biomedical ethicJ Med Ethics. 1995;21(6):332-338.
- Jecker NS. A broader view of justice. Am J Bioethics. 2008;8(10):2-10.
- Metzl JM, Hansen H. Structural competency: Theorizing a new medical engagement with stigma and inequality. Soc Sci Med. 2014;103:126-133.
- Wear D, Aultman JM. The limits of narrative: medical student resistance to confronting inequality and oppression in literature and beyond. Med Educ. 2005;39(1):1056-1065.